Uterine fibroids and polycystic ovary syndrome (PCOS) affect millions of women and often share symptoms that interfere with daily life. They can cause pelvic pain, irregular periods, and fertility problems. While these two conditions differ in cause and location, both can be managed effectively with early testing, medical care, and healthy lifestyle changes.
What Are Uterine Fibroids and PCOS?
Both uterine fibroids and PCOS influence reproductive health in unique ways. Knowing how they differ helps women choose the right tests and treatments.
Uterine Fibroids
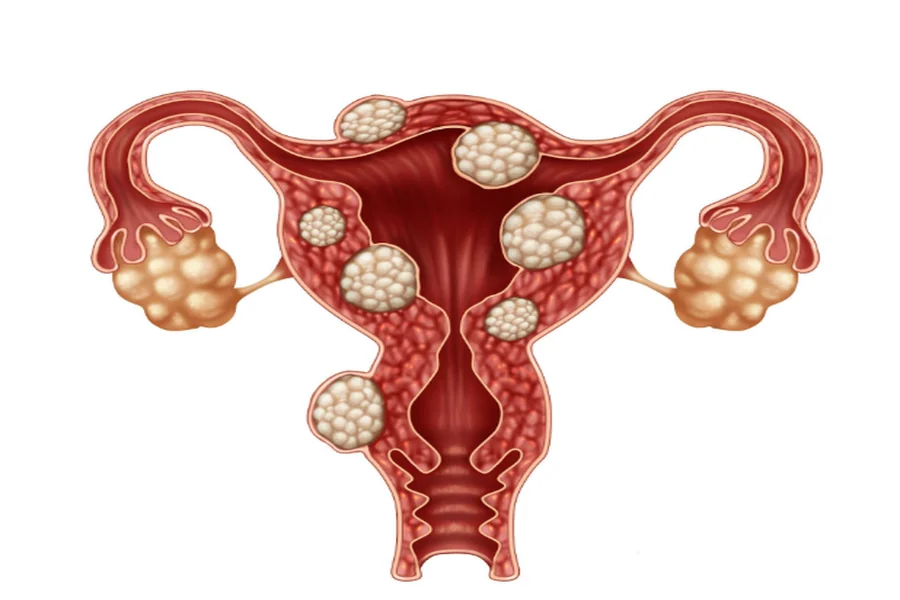
Uterine fibroids are noncancerous growths that form in or around the uterus. They can be small or large and may cause heavy bleeding, pelvic pressure, or lower back pain.
Up to 80% of women develop fibroids by age 50, and African American women are more likely to have severe symptoms. Hormone levels, family history, and lifestyle habits all affect their growth.
Polycystic Ovary Syndrome (PCOS)
PCOS is a hormonal disorder that affects how the ovaries work. It can cause irregular periods, high androgen levels, and small cysts on the ovaries. Women with PCOS may also experience acne, weight gain, or thinning hair.
How These Conditions Affect the Body
Fibroids and PCOS both disrupt normal reproductive function, often leading to changes in menstrual patterns and physical discomfort.
Menstrual Changes and Hormonal Shifts
Estrogen and progesterone control the menstrual cycle. When their levels change, problems arise. Fibroids tend to grow when estrogen is high, leading to longer and heavier bleeding. PCOS, on the other hand, causes skipped or unpredictable cycles due to irregular ovulation.
Tracking menstrual changes helps doctors pinpoint which condition may be responsible and guide treatment.
Pelvic Pain and Pressure
Fibroids can create pressure or fullness in the lower abdomen. Large fibroids may press against nearby organs, such as the bladder. PCOS can cause pain or bloating when ovarian cysts grow or rupture. For women dealing with persistent pelvic pain or heavy bleeding, procedures like fibroids in uterus treatment may offer long-term relief when medication alone isn’t enough.
If pain continues for weeks, doctors may suggest ultrasound imaging or MRI scans to see whether fibroids or cysts are present.
Reproductive Health Risks
Fibroids may block the fallopian tubes or affect the uterine lining, while PCOS interferes with ovulation. Both can make it harder to conceive. Over time, hormonal imbalance also increases the risk of endometrial cancer. Regular checkups help detect these issues early and protect fertility.
Diagnosis and Testing
Accurate diagnosis allows doctors to choose the right treatment plan for each condition.
Medical Evaluation
The process begins with a pelvic exam and a review of medical history. Doctors look for signs such as irregular bleeding, cramps, or abdominal pressure. Menstrual health care services offered at specialized clinics often include hormone profiling, imaging, and long-term monitoring. Blood tests are used to check hormone levels and insulin resistance, which often accompanies PCOS.
Imaging Procedures
An ultrasound is commonly used to identify fibroids or ovarian cysts. When more detail is needed, an MRI scan provides a clearer picture of the uterus and ovaries. These tests confirm the diagnosis and rule out other causes of pelvic pain.
Treatment and Management Options
Both fibroids and PCOS can be managed through a mix of lifestyle changes, medications, and, in some cases, procedures. The choice depends on symptoms and personal health goals.
Lifestyle and Home-Based Management
Healthy daily habits can make a noticeable difference. Doctors often recommend:
- Eating a diet rich in fruits, vegetables, and whole grains
- Staying active to regulate hormones and support weight control
- Reducing processed foods to lower inflammation
- Managing stress with yoga, meditation, or relaxation techniques
These changes help improve menstrual regularity and reduce fatigue or bloating.
Medical Treatments
Medication helps control symptoms and improve hormone balance.
- Hormonal birth control regulates cycles and lightens bleeding.
- Drugs that lower estrogen may reduce fibroid size.
- Insulin-sensitizing medicines, such as metformin, improve ovulation for women with PCOS.
Doctors adjust these treatments based on each woman’s progress and reproductive plans.
Minimally Invasive Procedures and Surgery
When medications aren’t enough, procedures may help. An interventional radiologist can perform uterine fibroid embolization, which blocks blood flow to fibroids so they shrink. In more serious cases, myomectomy or laparoscopic surgery may remove fibroids while preserving fertility.
Surgery for PCOS is less common but may help restore ovulation if other treatments fail.
Living With Uterine Fibroids and PCOS
Managing these conditions takes time and patience. Fatigue, irregular bleeding, and fertility worries can affect emotional health. Working with a gynecologist, nutritionist, or mental health professional provides steady support.
Support groups and online communities also help women share experiences and feel less alone. Regular follow-ups keep symptoms in check and prevent long-term complications.
Conclusion
Uterine fibroids and PCOS are common but manageable. Both require attention, consistent care, and healthy daily choices. Early testing and regular medical follow-ups help women protect their reproductive health and improve their quality of life.


